
The changing needs of your loved one at this stage
It is important to stay connected with the hospital’s palliative care team or the home hospice team looking after your loved one. They can offer guidance and support to help you during this challenging phase, as your loved one’s condition worsens. Given that his/her care needs may be different now, the palliative nurses/therapists can teach you how to safely carry out the following daily activities:
- Diaper change & skin care
- Wound care & dressings
- Transferring e.g. bed to chair
- Tube feeding
- Suctioning
- Any other day-to-day activities of concern
Some of these nursing skills can sometimes feel overwhelming to perform on your loved ones. There are available AIC Caregiver Training courses to help you learn and master these essential skills, and gain knowledge about palliative care.
To get the necessary medical equipment and devices, consult your loved one’s palliative team or you can refer to the list of useful contacts in this Caregiver Guide by Singapore Hospice Council. Additionally, you may want to explore the Equipment Rental Scheme for further assistance.
Due to your loved one’s condition, his/her food and fluid intake may need to be modified. Learn about the different types of diet modifications in Nutrition in Advanced Illnesses guide by Singapore Hospice Council.
Understanding the final hours
The period just before death occurs may range from the last few hours to a few days. Your loved one may start to show some of these physical signs:
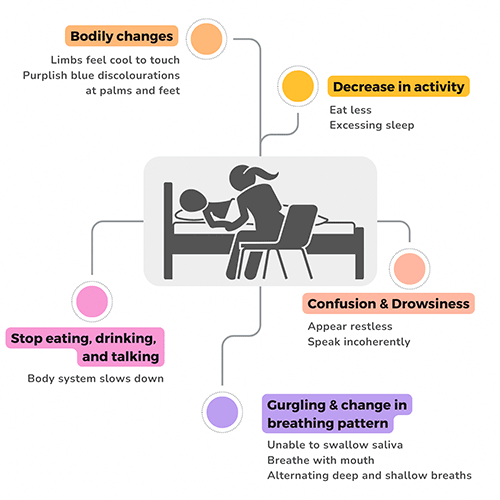
Source: Singapore Hospice Council
What can you do at the bedside?
Even when your loved one seems to be unconscious, he/she might still be able to hear you. Your loved one may take their final breath when you are not by the bedside. Learn to say goodbye whenever you have to leave his/her side. Share your love, gratitude with your loved one, and seek forgiveness from them in advance.
To know more on what you can do during your loved one’s final moments, refer to these guides published by Singapore Hospice Council:
